Reconstructive Pelvic Surgery
Reconstructive pelvic surgery refers to surgery that is meant to correct or "reconstruct" abnormalities of the pelvis without necessarily removing organs (the uterus, ovaries, fallopian tubes, etc.). There are two primary areas of RPS.
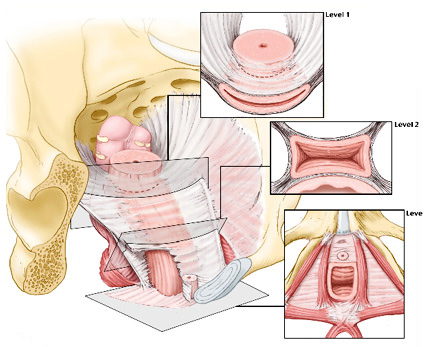
Uterine prolapse, urinary incontinence, and abnormalities of the pelvic floor (cystocele, rectocele, and enterocele) make up the first group of problems to which reconstructive pelvic surgery is directed. In these cases, there are specific defects in the structures supporting the vagina, bladder, uterus, and/or rectum that require "reconstruction". Sometimes, the uterus and/or ovaries are removed when this reconstruction is done, but it is not absolutely necessary.
Women with advanced endometriosis or adhesions from prior surgery (or both) who wish to retain their fertility constitute the second group of patients who might undergo reconstructve pelvic surgery. In these circumstances, the gynecologist must not only remove the endometriosis and treat all of the pelvic adhesions, but they absolutely must do it in such a way as to limit the chances of recurrence of the endometriosis and/or adhesions and , at the same time, maximize the patient's chances of attaining pregnancy. This can be a very difficult and tedious task that demands the highest levels of surgical skill and experience.


