Dr. Dibyendu Chakrabarty
MBBS (Cal.) DCH (Cal.) MD (Pediatrics) International Fellows of American Academy of Pediatrics (USA)

MBBS (Cal.) DCH (Cal.) MD (Pediatrics) International Fellows of American Academy of Pediatrics (USA)
A child's temperature can be taken from the rectum, ear, mouth, forehead, or armpit. It can be taken with a digital thermometer. Digital thermometers are easier to use and give much quicker readings (and usually give a signal when they are ready). Glass thermometers containing mercury are no longer recommended because they can break and expose people to mercury.

1) Rectal Temperatures are most accurate. That is, they come closest to the child's true internal body temperature. For a rectal temperature, the bulb of the thermometer should be coated with a lubricant. Then the thermometer is gently inserted about 1/2 to 1 inch (about 1 1/4 to 2 1/2 centimeters) into the rectum while the child is lying face down. The child should be kept from moving.
2) Ear Temperatures are taken with a digital device that measures infrared radiation from the eardrum. Ear thermometers are unreliable in infants under 3 months old. For an ear temperature, the thermometer probe is placed around the opening of the ear so that a seal is formed, then the start button is pressed. A digital readout provides the temperature.
3) Oral Temperatures are taken by placing a digital thermometer under the child's tongue. Oral temperatures provide reliable readings but are difficult to take in young children. Young children have difficulty keeping their mouth gently closed around the thermometer, which is necessary for an accurate reading. The age at which oral temperatures can be reliably taken varies from child to child but is typically after age 4.
4) Forehead Temperatures (temporal artery temperatures) are taken with a digital device that measures infrared radiation from an artery in the forehead (the temporal artery). For a forehead temperature, the head of the thermometer is moved lightly across the forehead from hairline to hairline while pressing the scan button. A digital readout provides the temperature. Forehead temperatures are not as accurate as rectal temperatures, particularly in infants under 3 months old.
5) Armpit Temperatures are taken by placing a digital thermometer in the child's armpit, directly on the skin. Doctors rarely use this method because it is less accurate than others (readings are usually too low and vary greatly). However, if caretakers are uncomfortable taking a rectal temperature and do not have a device to measure ear or forehead temperature, measuring armpit temperature may be better than not measuring temperature at all.
Warning signs
Certain symptoms are cause for concern. They include
• Any fever in infants less than 2 months old
• Lethargy or listlessness
• Ill appearance
• Difficulty breathing
• Bleeding in the skin, appearing as tiny reddish purple dots (petechiae) or splotches (purpura)
• Continuous crying in an infant or toddler (inconsolability)
• Headache, neck stiffness, confusion, or a combination in an older child
When to see a doctor
Children with fever should be evaluated by a doctor right away if they have any warning signs or are less than 2 months old.
Children without warning signs who are between 3 months and 3 years of age should be seen by the doctor if the fever is 102.2° F (39° C) or higher, if there is no obvious upper respiratory infection (that is, children are sneezing and have a runny nose and nasal congestion), or if the fever has continued more than 5 days.
For children without warning signs who are over 3 years of age, the need for and timing of a doctor's evaluation depend on the child's symptoms. Children who have upper respiratory symptoms but otherwise appear well may not need further evaluation. Children over 3 years of age with fever lasting more than 5 days should be seen by the doctor.

What the doctor does
Doctors first ask questions about the child's symptoms and medical history. Doctors then do a physical examination. A description of the child's symptoms and a thorough examination usually enable doctors to identify the fever’s cause.
Doctors take the child’s temperature. It is measured rectally in infants and young children for accuracy. The breathing rate is noted. If children appear ill, blood pressure is measured. If children have a cough or breathing problems, a sensor is clipped on a finger or an earlobe to measure the oxygen concentration in blood (pulse oximetry).
As doctors examine children, they look for warning signs (such as an ill appearance, lethargy, listlessness, and inconsolability), noting particularly how children respond to being examined—for example, whether children are listless and passive or extremely irritable.
Occasionally, the fever itself can cause children to have some of the warning signs including lethargy, listlessness, and ill appearance. Doctors may give children fever-reducing drugs (such as ibuprofen) and reevaluate them once the fever is reduced. It is reassuring when lethargic children become active and playful once the fever is reduced. On the other hand, it is worrisome when ill-appearing children remain ill-appearing despite a normal temperature.
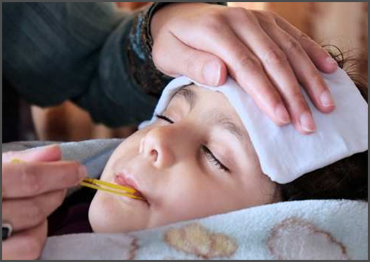
Treatment of Fever
If the fever results from a disorder, that disorder is treated. Other fever treatment focuses on making children feel better.
General Measures
Ways to help children with a fever feel better without using drugs include
• Giving children plenty of fluids to prevent dehydration
• Putting cool, wet cloths (compresses) on their forehead, wrists, and calves
• Placing children in a warm bath (only slightly cooler than the temperature of the child)
Because shivering may actually raise the child’s temperature, methods that may cause shivering, such as undressing and cool baths, should be used only for dangerously high temperatures of 106° F (about 41° C) and above.
Rubbing the child down with alcohol or witch hazel must not be done because alcohol can be absorbed through the skin and cause harm. There are many other unhelpful folk remedies, ranging from the harmless (for example, putting onions or potatoes in the child's socks) to the uncomfortable (for example, coining or cupping).
Key Points
• Usually, fever is caused by a viral infection.
• Infants under 2 months of age with a temperature of 100.4° F or higher need to be evaluated by a doctor.
• Children age 3 months to 3 years with fever who have no symptoms suggesting a specific disorder but look ill or have a temperature of 102.2° F (39° C) or higher need to be evaluated by a doctor.
• Teething does not cause significant fever.
• Drugs that lower fever may make children feel better but do not affect the disorder causing the fever