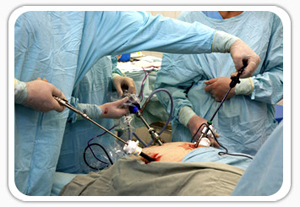
Treatment at a Glance

1) Routine Gynae & obstetrics Prepregnancy check up , Counselling High Risk Pregnancy, Pregnancy complicated with medical or other surgical complains.
2) Recurrent miscarriage Labour, delivery & Caesarean Section.
3) Operation for differnt tumours
4) Fibroids - Open / Lap myomectomy
5) Ovarian Cysts - Open / Lap cystectomy
6) Uterine Pathology - Hysterectomy, Abdominal, NDVH, TLH Non descent Vaginal Hysterectomy: where no mark is there from out side Operation is done through natural orifice.
7) Cosmetic Gynaecology: vaginoplasty, Breast enlargement or reduction.
8) But the best results are from Fertility Enhancing Surgeries see pictures above.
9) Urogynecology - Difficults in holding urine, leaking urine solved through TVT or TOT.
Treatment Provided

1) Laparoscopic Surgery
Laparoscopic surgery is also called “Minimally Invasive” surgery, which is a specific technique in the surgical procedure. It is used largely in gynecological surgery due to certain definite advantages. The laparoscope enables viewing of the area inside the abdomen during the surgery while the surgeon uses “trochars” for the surgical procedure. The surgical operation is done by looking at the monitor in the operation theater. The patient experiences lesser pain compared to the traditional surgery, gains in shorter recovery period and less scars on the abdomen. Most of gynecological surgeries can be performed through laparoscopic surgery, which is definitely safer than the conventional method because of the smaller incision.
All kinds of high-risk obstetric cases are undertaken by the best laparoscopic surgeon in Kolkata, which includes advanced laparoscopic procedures such as,
• Total Laparoscopic Hysterectomy
• Laparoscopic Myomectomy (removal of tumor from uterus), retaining and reconstructing the uterus
• Laproscopic removal of ectopic pregnancy.
• Laproscopic removal of dermoid cyst.
• Laproscopic surgery for the endometriosis
• Laparoscopic surgery for the infertility patients
• Laparoscopic surgery for the genital prolapsed and stress incontinence
• Laparoscopic treatment for genital tuberculosis
• Tubal reconstructive surgery
• Laparoscopic surgery of ectopic pregnancy
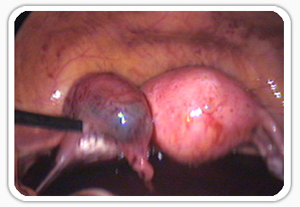
Acute Ectopic Pregnancy
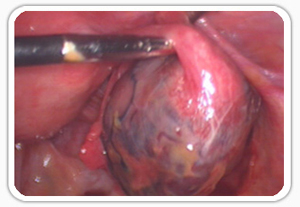
Chronic Ectopic Pregnancy
2) Hysteroscopic Procedures
• Diagnostic hysteroscopy procedure
• Tubal cannulation for blocked tube
• Hysteroscopic tubal cannulation for blocked fallopian tube.
• Hysteroscopic removal of polyps and myomas
• Hysteroscopic removal of uterine septum
• Hysteroscopic treatment of uterine synechiae.
• Complete evaluation of infertility couples include procedures like,
• Medical treatment of infertility
• Surgical treatment of infertility (avoiding invitrofertilization/test tube baby).
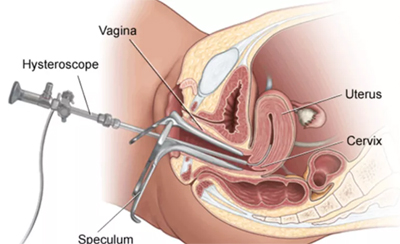
3) Infertility Management
Fertility problems are easily diagnosed and treated by the infertility specialist in Kolkata for women of advanced ages or over the age of 35. Though the chances of getting pregnant are reduced with each passing year, the recommendation of the specialist doctor brings delight to numerous women desiring to become mothers. However, no treatment can guarantee a baby, but you should contact the best gynecologist in Kolkata so that you stand a very good chance in conceiving. You have to comply with a plan along with your partner to make the treatment successful. You can surely achieve the desired results at a cost, which you would certainly be able to afford.

4) Urogynaecology
Urogynaecology covers the medical management of urinary problems and pelvic disorders in females, which are fairly common in women, but are not discussed due to certain stigmatic observations. The condition is associated with loss of urine control, bowel symptoms, and pelvic discomfort and so on and especially in aged females, which remain undiagnosed and untreated. The condition is well treated by the specialist gynecologist in Kolkata ushering new hopes for suffering ladies.
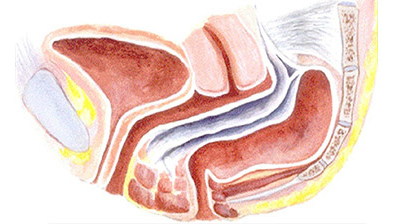
5) Geriatric Gynecology
With the increase in age, women become vulnerable to a number of gynecological problems, which need proper treatment from a specialist gynecologist. Certain health issues may impede the normal lifestyle of aged women such as sensory deficits, physical disability, cognitive impairment, uterine incontinence, etc. which need sophisticated medical care by consultant gynecologists.
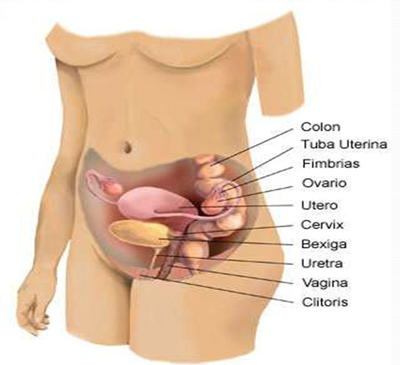
6) High Risk Pregnancy Care
The high-risk pregnancy condition is adjudged when there are complications jeopardizing health of the baby or the mother or both. It needs to be managed by a consultant obstetrician and gynecologist in Kolkata to ensure favorable conditions for the baby and the mother. The situation may develop due to various factors including maternal age, medical health conditions before the pregnancy, etc.
High risk pregnancy is a team work. I have an excellent team of physician, endocrinologist, cardiologist, and dietician etc. to efficiently combat each & every case.

7) Recurrent Miscarriages
Common symptoms include light to heavy vaginal bleeding constantly or intermittently. Though there may be sporadic bleeding in the first trimester of pregnancy, but the bleeding associated with pain may indicate higher chances of miscarriage. Persistent abdominal pain, pelvic cramps, lower backaches are some of the signals. Many females experience passing of vaginal blood clots. The miscarriage condition can only be properly evaluated by a specialist gynecologist because of variation of experiences of different females.
There are 1001 causes for recent miscarriage. Evolution of cause and individualization of treatment in the key to success. I have treated a lady who had 8 miscarriages and 9th baby was deliverd by me.

8) Treatment of heavy Bleeding
The medical term for abnormal or prolonged or heavy bleeding is Menorrhagia. It is a common symptom in pre-menopausal women, which may result in anti-emetic condition of women. Symptoms include soaking of pads or tampons hourly for several hours. Many may need double napkins to achieve control over the condition, waking up in the night to change sanitary protection due to excessive bleeding and so on. Lifestyle is harshly impaired with signs of anemia, tiredness, fatigue, breath loss and irritability, etc

9) Cosmetic Vaginal Surgery
It is a combination of labiaplasty and vaginoplasty surgical procedures. The vaginal rejuvenation is done to improve the look and functioning of the organ. It is mainly performed to improve the cosmetic appearance of the organ to regain confidence and self esteem. Labiaplasty concerns the reduction of the size and alteration of the shape of the vagina, which is required by women born with the defect. Vaginoplasty related to the tightening of the vagina and surrounding muscles to experience improved satisfaction during sexual activity. It may also be requisitioned after the delivery of the baby affecting the appearance of the vagina. The treatment of torn hymen is termed hymenoplasty, which may happen during sexual intercourse or by accident. The specialist laparoscopic surgeon in Kolkata is able to offer the best services in this respect in total confidence.

10) Menopausal Problems
All females experience the condition of menopause when they reach a certain age. Common symptoms include mood variations, urinary incontinence, night sweats, sleep problems, sexual discomfort, hot flashes, etc. Symptoms are associated with emotional distress, which should be controlled and tackled properly. The lifestyle of the midlife woman is affected seriously and here, you should approach a specialist gynecologist in Kolkata to obtain relief in the situation by discussing your concerns and acquiring proper consultation in this respect.
The menopause is sometimes known as the 'change of life' and is marked by the ending of menstruation (when a woman's periods stop). In india the average age of menopause is 51 yrs. A woman is said to have become menopausal once she has not had a period for one year. When menopause occurs under 45 years of age, it is known as premature menopause. It is estimated that premature menopause affects 1% of women under the age of 40 and 0.1% of women under the age of 30.
As the ovaries now produce less estrogen, many women experience both physical and emotional symptoms, such as hot flushes, night sweats and irritability. These symptoms may last for about 2-3 years after menopause. For women who find the symptoms interfering with quality of life, hormone therapy (HT) may provide significant relief. Hormone therapy is commonly also known as Hormone Replacement Therapy (HRT), but the latter term is less accurate.
HT comprises of low dose estrogen and progestogen to alleviate symptoms of menopause. In addition it has a protective effect on bone density and on colon cancer. The risks of prolonged HT are increased risks of stroke and thrombosis, of breast and possibly ovarian.
It is recommended that the smallest possible dose of HT be prescribed for a short duration to achieve the benefits without increasing unduer risks of thrombosis and cancer.
I run a menopausal clinic where each and every problem of a menopausal patient are identify, discuss and effectively treated.
Hormone therapy is available as tablets, skin patches, gels and creams. Tablets and skin patches aim to act upon the entire body, whilst gels and creams are aimed for a more local effect. For more information please visit the Indian Menopause Society website.

11) Family Planning & Contraception
Family planning is achieved through contraceptive procedures to avoid pregnancy. The main task of contraception is to offer effective protection in this respect so that pregnancy does not transpire even after conjugal intercourse. You need to discuss with the obstetrician and gynecologist in Kolkata to obtain complete protection by using different methods of contraception such as pills, barriers, implants, injection, permanent contraception, etc. The choice depends on the age, health status and need. The specialist gynecologist would be able to recommend the best method for you.
Contraception is the use of hormones, devices or surgery to prevent a woman from becoming pregnant. It allows women to choose when and if they want to have a baby.
The male condom is the only type of contraception that also protects men and women from sexually transmitted infections (STIs).
There are several types of contraception which work in different ways.
Condoms create a physical barrier against fertilisation.
Hormonal methods for women, such as the contraceptive pill, prevent the release of an egg from the ovaries and change the environment of the womb to prevent pregnancy.
Contraceptive devices, such as the IUD (intrauterine device), are placed in the womb and prevent pregnancy by releasing copper or hormones into the wom
Two newer methods of contraception have been received well by women.
1) Intra-uterine system (IUS).
This is a small T shaped device containing progestogen (synthetic form of the natural hormone progesterone) inserted into the uterus where it releases small amounts of the hormone continuously. It is a long lasting and reversible method of contraception. The hormone makes the lining of the womb thinner so it is less likely to accept a fertilised egg, thus preventing pregnancy. It also thickens the mucus from the cervix (opening of the womb), making it harder for sperms to move through it and reach the egg. In some women, the IUS also stops the ovaries from releasing an egg, but most women will continue to ovulate. The IUS available in the UK is called Mirena and works for up to five years after insertion. If fitted at age 45 yrs or over it can be left until menopause is reached. The IUS is over 99% effective in preventing pregnancy, and removal of the device restores fertility
2) Contraceptive implants
The contraceptive implant is a long-acting, effective method of contraception. It is over 99% reliable in preventing pregnancy. It works by slowly releasing progestogen into the body. It can be started at any time during the menstrual cycle after excluding pregnancy. There is currently only one type of contraceptive implant available in the UK called Implanon. It is a small (4cm), thin flexible tube implanted under the skin of the upper arm by a doctor or nurse, using a local anaesthetic to numb the area. The small wound made in the arm is closed with a dressing and does not need stitches. Implanon works for up to three years before it needs to be replaced, and can be continued until menopause. The implant can be removed at any time by a specially trained doctor or nurse. It takes a few minutes to remove, using a local anaesthetic. However, the contraceptive effect stops immediately with removal of the implant.
I run a menopausal clinic where each and every problem of a menopausal patient are identified, diecussed and effectively treated.

12) Fetal Medicine
The consultant gynecologist is qualified to offer help to female patients with fetal medicines in high-risk pregnancy situations such as in the pregnancy with twins. You should call on the high-risk pregnancy doctor in such conditions of pregnancy to obtain appropriate medical treatment.
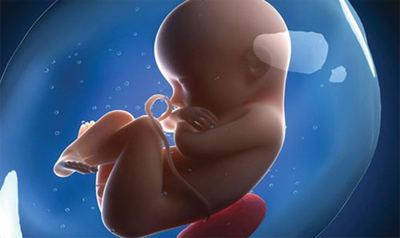
13) Counseling Services
Counseling services offer a wide range of healthcare recommendation to females for safe and comfortable living. Professional experts and experienced gynecologists in Kolkata provide all possible help to women on several of issues including choice of contraceptives, pregnancy options and in infertility symptoms and others in confidential atmosphere.

14) Down's Syndrome Screening
What is Down’s syndrome?
Down’s syndrome is a chromosomal defect caused by the presence of an extra copy of chromosome 21. Down’s syndrome has a wide range of manifestations and is predominantly characterised by mental retardation of varying severity and unusual facial characteristics. Often, there are other associated problems in individuals with Down’s syndrome.
Anyone can have a pregnancy affected by Down syndrome, but the risk increases with advancing mother’s age. The risk increases from 1:1350 at age 25yrs to 1:350 at age 35yrs, and to 1:85 at 40yrs.
The condition is usually sporadic and does not run in families. However, if a mother has had a pregnancy affected by Down’s syndrome, her risk of Down’s syndrome in a subsequent pregnancy would be higher.
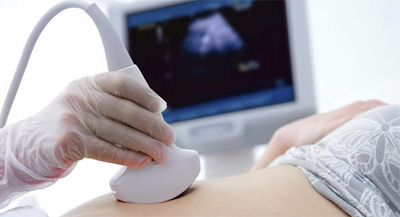
Screening for Down’s syndrome:
All pregnant women should be offered screening for Down’s syndrome on the NHS (FASP). Screening, as recommended by the NHS, should comprise of nuchal scan and blood tests at 11 to 13+6 weeks of pregnancy. All measurements and other risk factors are entered into a complex mathematical calculation to determine the person’s individual risk for Down’s syndrome.
The individual risk (eg your own risk) for Down’s syndrome is given as a figure, also supported by a qualifying phrase as ‘low risk’ or ‘high risk’. The cut-off point for ‘high risk’ varies according to which test is applied. Women at low risk for Down’s syndrome are not offered further testing on the NHS.
For those deemed as high risk, discussion with a fetal medicine expert is recommended so that options of conservative management or invasive tests, and the risks thereof, are discussed so that the most appropriate choice may be made for the individual and her family.
For those who are at ‘high risk’ for Down’s syndrome or those who are anxious about the risk of Down’s syndrome and wish for a definitive answer, either of the two following invasive tests is available for diagnosis. The appropriateness of the test depends upon the weeks of gestation.
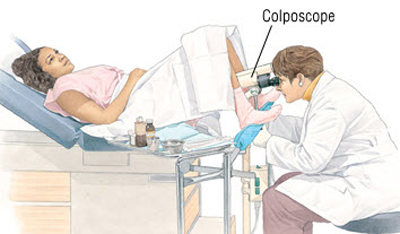
15) Colposcopy
Colposcopy is a diagnostic procedure to examine an illuminated, magnified view of the cervix and the tissues of the vagina. A colposcopic examination follows an abnormal cervical smear report. An abnormal smear report may be described as :
Mild changes in the cells (mild dyskaryosis)
Moderate changes in the cells (moderate dyskaryosis)
Severe changes in the cells (severe dyskaryosis)
An abnormal smear report indicates that there are precancerous changes in the cells covering the cervix, and requires further investigations using a colposcope. Many premalignant and malignant lesions on the cervix have detectable characteristics which can be identified through the colposcope, and biopsies taken for pathological examination.
Colposcopy is an outpatient procedure performed with the woman lying on her back, legs in stirrups, and buttocks at the lower edge of the table (a position known as the dorsal lithotomy position). A speculum is inserted to open the vagina so that the cervix at the top can be seen. The colposcope is a microscope that is placed outside the speculum (and outside the body) and the cervix visualised. Special dyes are used to paint the cervix to demonstrate any abnormal appearing areas. The dyes commonly used are acetic acid and iodine. It is very important to visualise an area on the cervix called the transformation zone where most of precancerous and cancerous lesions arise.
Areas of the cervix which turn white after the application of acetic acid or have an abnormal vascular pattern are abnormal, and application of iodine helps in highlighting these areas as they do not take the dark brown stain of the iodine. Colposcopic assessment classifies the lesion as low grade and high grade.
After a complete examination, the areas with the highest degree of visible abnormality are defined and biopsies obtained. Most doctors and patients consider anesthesia unnecessary, however, a local anaesthetic may be used to diminish patient discomfort, particularly if more than one biopsy samples are taken. The raw areas after biopsy are touched with silver nitrate sticks to control bleeding. Women can expect to have a thin grey discharge for up to several days after the procedure.
Pathology
Abnormalities on the biopsy samples are then described as:
• CIN 1 - one third of the thickness of the lining covering the cervix has abnormal cells
• CIN 2 - two thirds of the thickness of the lining covering the cervix has abnormal cells
• CIN 3 - the full thickness of the lining covering the cervix has abnormal cells
Treatment:
Without proper treatment, precancerous abnormalities may develop into cancerous lesions. Various treatments exist for significant lesions, most commonly loop excision of transformation zone (LLETZ), and knife cone excision. All treatment procedures aim to remove or destroy the abnormal cells.
LLETZ is the shortened name for the procedure Large Loop Excision of Transformation Zone. It is an outpatient procedure and the person undergoing the procedure can go home later. The procedure involves removing the transformation zone on the cervix bearing the abnormal cells by using a thin metal wire shaped like a loop through which an electric current is passed.- an electrosurgical technique. The procedure is done under local anaesthesia under colposcopic guidance. However for very anxious women or where the procedure is expected to be difficult, it may be appropriate to be done in operating theatres and under a general anaesthetic.
Follow up
Appropriate follow-up after treatment is very important. Follow-up is done by regular cervical smears starting at 6 months after treatment. For those who have had CIN 2 or worse should have annual smears for 10 years. Women treated for CIN1 can return to routine screening after 2 years of negative smears.
16) Cervical Screening
The Well Woman Screen aims to offer core assessment of the health and well being of our patients. We have chosen 4 areas of important health checks which includes screening for cervical cancer and ovarian cancer, and advice on contraception and hormone therapy in menopause.
• Cervical Screening
• Ovarian Cancer Screening
• Advice on Contraception
• Menopause and Hormone Therapy
Cervical screening aims to identify at risk women and to prevent cancer of the neck of the womb (cervix) by detecting and treating early abnormalities. If these abnormalities remain undetected they could lead to cervical cancer over a period of time.
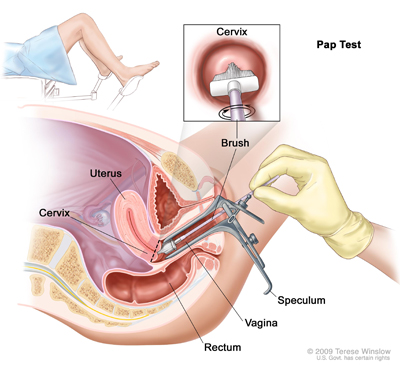
Cervical screening tests do not give a diagnosis but indicate risk. Regular screening reduces the risk of cervical cancer by 90%. Cervical screening is performed by taking scrapings from the neck of the womb using a soft brush and collecting these scrapings in either of two liquid media, Thinprep or Sureprep. This method of screening called LBC (liquid based cytology) has now completely replaced the old technique of using a wooden spatula and smearing the scrapings on a glass slide. LBC is more accurate with lower false negative results. It also gives the additional benefit of testing for human papilloma virus (HPV) and the type.
The procedure is not painful, but may be uncomfortable.
Screening on the NHS starts at 25 by invitation, and is then at 3 yearly intervals between the years of 25 to 49 and 5 yearly from age 50 to 64 (NHS cervical screening programme).
Earlier and more frequent screening is available in the private sector, as is the option of HPV testing and typing. There are about 100 types of wart viruses, of which types 16, 18, 31, 33 and 45 are more associated with cervical intra-epithelial neoplasia (CIN) and invasive cancer.
On detection of abnormal cells, referral for colposcopy would become necessary. creening is looking for cancer before appearance of any symptoms and can help detect and treat cancer at an early stage. Often by the time symptoms appear, cancer may have begun to spread, and treatment becomes much more difficult.
For any screening to be effective, there must be an accurate test to use. And the test must be reliable enough to detect cancer or pre-cancer and also must not give false positive results in those who do not have cancer.
At the moment, there is no screening test that is accurate and reliable enough to detect ovarian cancer in the general population. But there are clinical trials going on looking into screening (eg UKCTOCS), and we will need to await the results of these trials.
Tests that are being studied as screening methods for detecting ovarian cancer in the general population are:
Transvaginal ultrasound of the ovaries to look for ovarian size and any cysts CA125 measurement in the blood. CA125 is a protein that is found in high amounts in the blood of patients with certain types of cancer including ovarian cancer. CA125 is also used in monitoring response of cancer to treatment.
Screening women at higher risk
Higher than average risk means having 2 or more relatives on the same side of the family diagnosed with ovarian cancer or breast cancer at a young age. Screening using transvaginal ultrasound and blood tests for CA125 is indicated in these high risk women. However, these screening tests have not been fully evaluated yet, and there is no guarantee that they will pick up every case of early ovarian cancer.
17) SEX REASSIGINING SURGERY
Female to Male transformation surgeries done in association with team of renowned Plastic Surgeons.